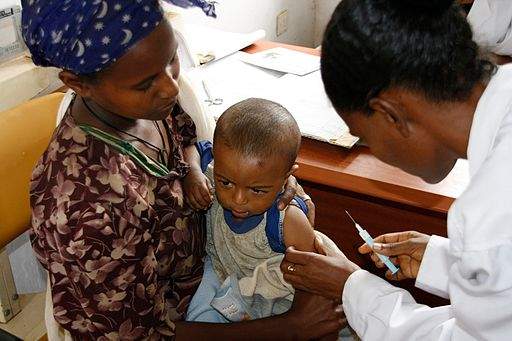
Wednesday 25 April marks the World Health Organization’s (WHO) tenth annual World Malaria Day, with this year taking the theme ‘Ready to Beat Malaria’.
The awareness day represents a time for drug developers and researchers from across the globe to come together and assess the progress made in tackling one of the world’s oldest and deadliest diseases, as well as the challenges still faced. NGOs and commercial businesses take the day as a chance to pledge money towards malaria interventions, while fundraising events are held in support of treatment and prevention programmes.
In celebration of this year’s event, Nigeria-based firm Superior Pharmaceuticals has announced it will be distributing its malaria treatment Sumether for free. The treatment is an artemisinin-based combination therapy (ACT), which sees artemisinin-based compounds combined with a drug from a different class, in this instance the drugs artemether and lumefantrine. Sumether is recommended by WHO as a first-line treatment for malaria patients.
Nigeria, and other countries including Chad, Niger and Mali, experience malaria transmission that is seasonally dependant. As such, treatments become particularly important during the upcoming rainy season, which is known to increase the spread of mosquito parasites. Nigeria currently has the highest proportion of malaria cases in the world, making up 29% of global malaria infections.
As no alternative to artemisinin is anticipated to enter the drug development market for several years, the necessity to preserve ACTs’ efficacy is crucial. However, these efforts have been threatened by an increasing resistance to antimalarial medications, which has long been recognised as an obstacle to eliminating the disease and which has been highlighted in various studies.
In a study presented at the Pan African Malaria Conference on the week of 16 April, researchers estimated that 21.3 million malaria patients in endemic African countries receive doses of ACT that are too low to be effective. This poses a problem as if initial treatment does not eliminate the malaria parasites in patients, the remaining infection can mutate and become resistant to future treatments.
How well do you really know your competitors?
Access the most comprehensive Company Profiles on the market, powered by GlobalData. Save hours of research. Gain competitive edge.

Thank you!
Your download email will arrive shortly
Not ready to buy yet? Download a free sample
We are confident about the unique quality of our Company Profiles. However, we want you to make the most beneficial decision for your business, so we offer a free sample that you can download by submitting the below form
By GlobalDataEndemic countries additionally see a prevalence of poor quality antimalarial medications, another contributing factor in the growth of antimalarial resistance.
Another study conducted by the Infectious Diseases Research Collaboration and presented at the same conference highlighted the problem of over-prescription. The researchers found ACT prescription for patients with negative malaria test results was prevalent, while a KEMRI-Wellcome Trust study found hospitals in Western Kenya commonly gave malaria treatments to children who had tested negative for malaria.
To maintain the efficacy of malaria medications, WHO has recommended treatments only be adopted if they have a cure rate of more than 95%, which should be monitored at least once every two years. Additionally, it suggests resistance-prone areas add more sentinel sites to enable more rapid identification of new resistance foci.
Moves to simplify the diagnostic process are also underway, in an effort to tackle such problems. Earlier this week PATH and UK-based test developer Mologic announced their partnership for a new, rapid diagnostic test (RDT) for relapsing, or plasmodium vivax, malaria (p.vivax).
The novel G6PD RDT will be designed to assist the safe and appropriate administration of primaquine, part of a class of drugs known as 8-aminoquinolines which are currently the only means of treating the p.vivax strain of the illness. It will also be designed for use at community level–where the majority of malaria diagnoses and treatments occur–through providing a simple positive or negative result in the determination of whether a patient has a risk of side effects if treated with primaquine.
Malaria is transmitted through the bites of infected female Anopheles mosquitoes and is caused by plasmodium parasites. There are five parasite species which cause malaria in humans, with the two most common being plasmodium falciparum and plasmodium vivax. The former is the most common form of the parasite in Africa, while the latter is the most common form in countries outside of sub-Saharan Africa.







