Clinical depression represents a major public health challenge whose diagnosis and treatment are frequently hindered by social stigma or patient reticence to seek care. Among the countries contending with the challenge of depression care is Germany, where its lifetime and 12-month prevalence remain high. In the March 2026 publication of The Lancet Regional Health – Europe, Elisabeth Schramm and colleagues explored the potential of digital counselling methods to reduce depression symptoms among patients, as well as signs of mental distress among caregivers. Their findings indicate that novel digital interventions may have results similar to those of status quo treatment methods, paving the way for other explorations of digital mental healthcare. GlobalData epidemiologists forecast that between 2026 and 2029, the 12-month total prevalent cases of major depressive disorder will decline from 5.62 to 5.48 million. Expanding treatment options to digital platforms such as those detailed by Schramm and colleagues may allow for expanded counselling options for these patients and their caregivers, while also reaching populations previously unable to receive mental health support.
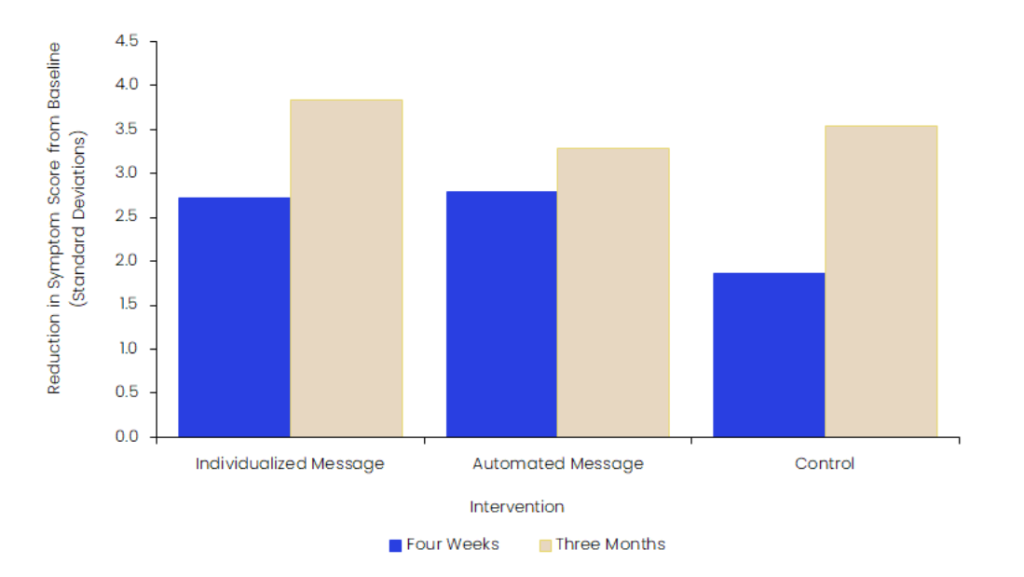
Schramm and colleagues conducted a randomised controlled trial among 1,640 adult participants throughout Germany who were either diagnosed with depression or who were caregivers of an individual with diagnosed depression between 2020 and 2024. The participants were split into three cohorts: one receiving individualised support messages produced by trained psychologists, another receiving automated support messages, and the final receiving standardised information material with no regular support messages. To gauge the impact of these scenarios, the authors administered online surveys pre- and post-intervention that measured psychological distress using the Kessler Psychological Distress Scale or the presence of depression symptoms using the Patient Health Questionnaire, depending on whether participants were caregivers or depression patients. As shown in Figure 1, the individuals enrolled in the individualised and automated support program showed a significant reduction in signs of personal distress, declining from baseline signs of distress at standard deviations (SD) of 2.68 and 2.53, respectively, at three months of intervention. By contrast, the control group showed a decline of only 1.50 SD in mean score. However, among patients with depression, the authors observed a 3.84 and 3.28 SD decline in depressive symptom scores for the individual and automatic messages compared to a decline of 3.54 among control group participants (Figure 2). This suggests that individualised and automated messages may lead to improvements in depression symptoms, but at a comparable level to treatment as usual.
The findings of Schramm and colleagues show mixed results, but promising signs for the future of mental healthcare. For caregivers and patients with depression alike, an expanded selection of programs showed a viable, effective pathway to a reduction in signs of mental distress. Similarly, although there were no significant differences in symptoms between treatment as usual and online support messages, their effects were comparable across cohorts. Provided that similar findings are obtained from other trials, the authors’ results may provide a rationale for expanded online care for depression. Expanded treatment options through virtual care can enable a wider array of treatments for patients and caregivers, especially those with limited access to mental health support, such as individuals living in rural settings or unable to afford regular in-person care. While further exploration is needed to validate results, such studies build the case for digital innovation as a vehicle for improvement in mental healthcare equity.
Figure 1: Reduction in symptoms of mental distress, ages ≥18 years, men and women, 2020─24, standard deviations
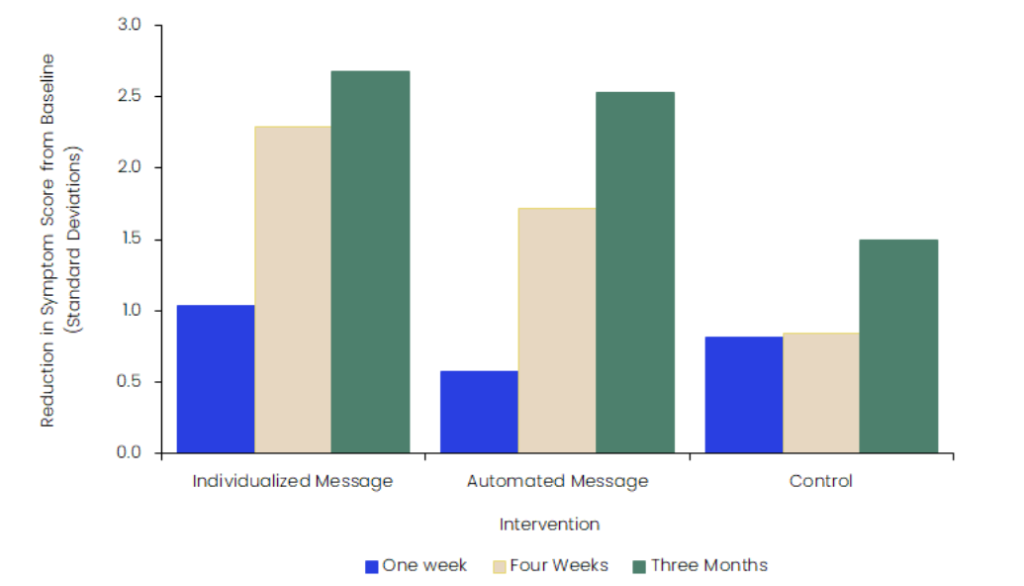
Figure 2: Reduction in symptoms of depression, ages ≥18 years, men and women, 2020─24, standard deviations