A longstanding aim of the cancer research community has been to increase the body’s ability to respond to cancerous cells.
The rationale is that a robust immune response to cancer would be sufficient to rid the body of tumours and cancerous cells that remain following pharmacological or surgical interventions.
We are finally beginning to see positive results, with the success of CAR-T therapies in leukaemia and the recent news that a woman was cured of metastatic breast cancer following a similar procedure.
Drugs, Tech, or both?
A GBI Research report due to be published this month has identified several promising breast-cancer pipeline targets that work as immunotherapies.
This is reflective of several factors, the first factor being the high revenues some immunotherapies have achieved within the breast cancer treatment algorithm and the second is that these drugs have been shown to extend life for cancer patients consistently and have the potential to promote an immune response great enough to rid the body of cancer.


US Tariffs are shifting - will you react or anticipate?
Don’t let policy changes catch you off guard. Stay proactive with real-time data and expert analysis.
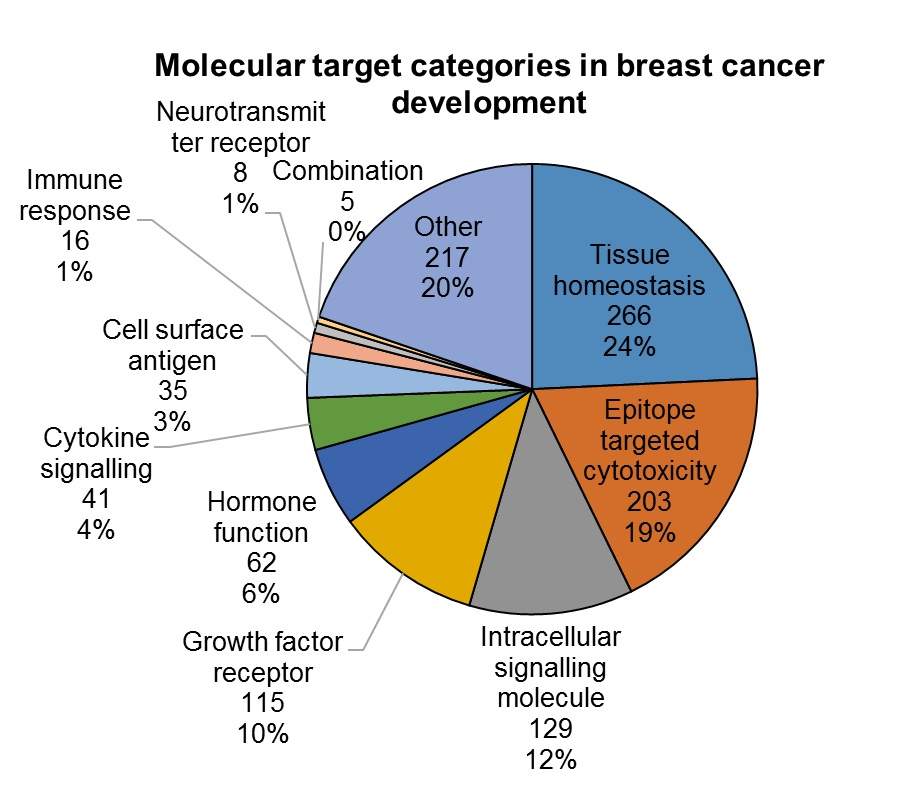
By GlobalDataDespite having a small presence in the pipeline with less than 1% of drugs targeting the immune response directly and only 4% targeting cytokines, molecules that are involved in the immune recognition of cancer cells occupy three of the top five spots in GBI Research’s assessment of promising molecular targets.
CAR-T
CAR-T therapy is a kind of immunotherapy that has been used in the treatment of a severe treatment-resistant leukemia.
It works by genetically modifying the patient’s own T-cells to carry antibodies that enable these cells to find and destroy cancer before re-injecting them into the blood stream.
CAR-T only needs to be used once and the effects are thought to be lifelong
Novartis’s Kymriah, the most widely known CAR-T therapy, costs $400,000 and is successful 80% of the time, with the remaining 20% of patients being offered refunds.
A relatively cheap, curative cancer treatment such as this is the dream of patients, insurers and healthcare systems alike, although CAR-T technology itself is yet to be applied successfully to solid tumors.
TIL therapy
TILs are cells which are capable of detecting tumor cells and attacking tumors but are neither strong enough nor found in sufficient number to destroy tumors.
A new therapy that involves isolating TILs, cloning them until they number into the billions and then reinjecting the strongest cells alongside the immunotherapy drug pembrolizumab managed to cure a breast cancer patient whose disease was considered terminal.
This strategy is yet to be tried in greater cohorts of people, and researchers worry that not all patients will have sufficient TILs in their tumours.
Nonetheless, this is an extremely promising breakthrough and the first time an immunotherapy technology has been able to entirely cure a person with a solid tumour.
Hard work pays off?
That immunotherapy technologies have cured both solid and blood-borne cancers is encouraging.
Although TIL therapy for breast cancer is still in its infancy, the early success of this approach combined with better pharmacological treatments and attempts to develop CAR-T technologies for solid tumours points to a bright future in cancer treatment for patients and medical professionals alike.