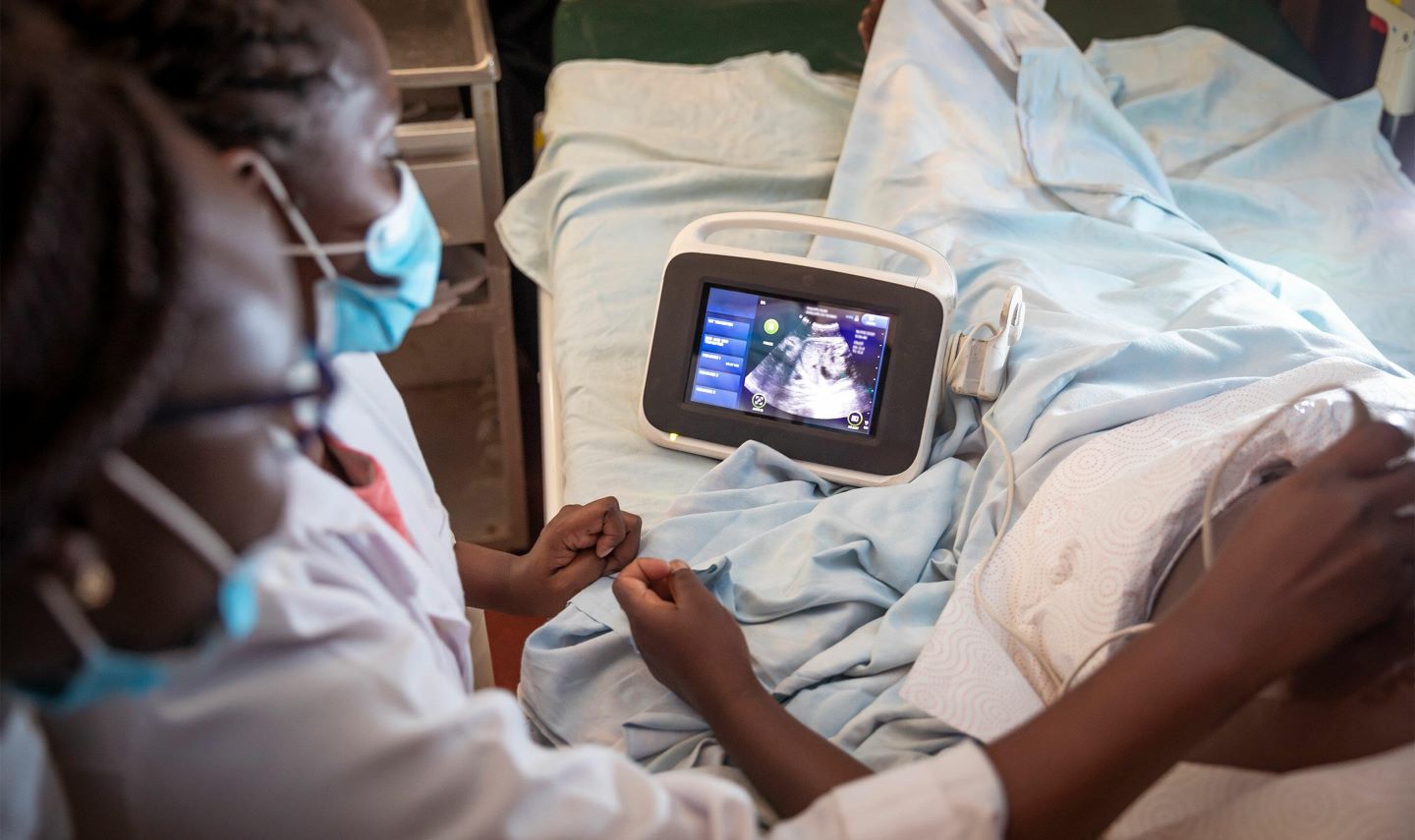
The Liverpool School of Tropical Medicine (LSTM) in Liverpool, UK, has reported that a new combination therapy could reduce the risk of malaria in pregnant women living with human immunodeficiency virus (HIV).
The finding comes from the IMPROVE-2 study, which assessed the addition of a monthly dose of the antimalarial drug dihydroartemisinin–piperaquine to co-trimoxazole administered daily.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The study is a collaborative effort involving LSTM, the Kenya Medical Research Institute, the Kamuzu University of Health Sciences and the Malawi University of Science and Technology.
It enrolled 904 subjects, who were randomly assigned to receive either the new drug combination or the standard care of daily co-trimoxazole alone.
According to the findings, a 68% reduction in malaria cases during pregnancy was reported in subjects who received the combination treatment versus those in the standard care arm.
The data indicate that the combination of dihydroartemisinin–piperaquine and daily co-trimoxazole could ‘substantially reduce’ the risk of malaria in pregnancy.
The research is part of a series of LSTM-coordinated trials, which aimed to find alternative malaria prevention methods for pregnant women, including those without HIV.
Dihydroartemisinin–piperaquine emerged as the only antimalarial drug observed to be well-tolerated to be considered for this purpose.
The recommended malaria prevention for pregnant women with HIV to date was a daily dose of co-trimoxazole, which also serves to prevent opportunistic infections in HIV patients.
Despite this, the rise in resistance to drugs such as co-trimoxazole among malaria parasites has been a cause for concern and has highlighted the need for alternative treatments.
Liverpool School of Tropical Medicine Tropical Epidemiology professor Feiko ter Kuile said: “These are promising findings, and potentially welcome news in the future of prevention [of] malaria among pregnant women living with HIV in areas where prevalence of the disease is high.”





