A recent study presenting a new understanding of the underlying biology of bipolar disorder (BD) could offer hope that new and more effective treatment could be developed.
The study was conducted by the Universidade Federal do Rio Grande do Sul (UFRGS) in Brazil, the University of Arizona College of Medicine in the US and McMaster University in Canada.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
The resulting article, called ‘EGR3 immediate early gene and the brain-derived neurotrophic factor in bipolar disorder’, was published on 5 February 2018 in the journal Frontiers in Behavioral Neuroscience. It explores BD patients’ difficulty responding to environmental stimuli such as stress, and its link with their impaired cellular resilience.
Bipolar disorder research
Environmental and genetic factors have long been known to play a crucial role in the development of BD. In particular, it has been associated with prolonged exposure to high levels of stress, especially during childhood.
Emotional stimuli, such as stress, transiently activate the response of genes known as immediate early genes (IEGs). As a reaction to a stressor, IEGs trigger the process of neuronal plasticity, during which the brain’s cells change their form and function. In so doing, the brain is able to learn from and adapt to new experiences.
The rapidity with which IEGs react to stimuli makes them of great interest to the field of psychiatry, and a potential target for future BD medication.
IEGs produce a type of protein known as the early growth response (EGR) protein, which turns environmental influences into long-term changes in the brain. These are mostly produced in response to stress and sleep deprivation. Without them, brain cells and the brain itself cannot respond appropriately to the numerous environmental stimuli received.
Neuronal plasticity also depends on neurotrophins – regulatory factors that help the development and survival of brain cells. The neurotrophin found most in the brain is brain-derived neurotrophic factor (BDNF).
Some studies have shown that levels of BDNF in BD patients diminish during periods of depression, mania or hypomania. Other studies show that BD patients have reduced levels of BDNF regardless of mood. However, overall it seems that changes in BDNF levels are a characteristic of BD patients, something that may contribute to the pathophysiology of the disease.
A 2016 study found that BD patients do not show a normal response to stress or environmental changes, having more difficulty coping with them than healthy individuals. One type of IEG known as EGR3, which responds to environmental changes and stress, was found to be repressed in the brain of BD patients.
The key findings
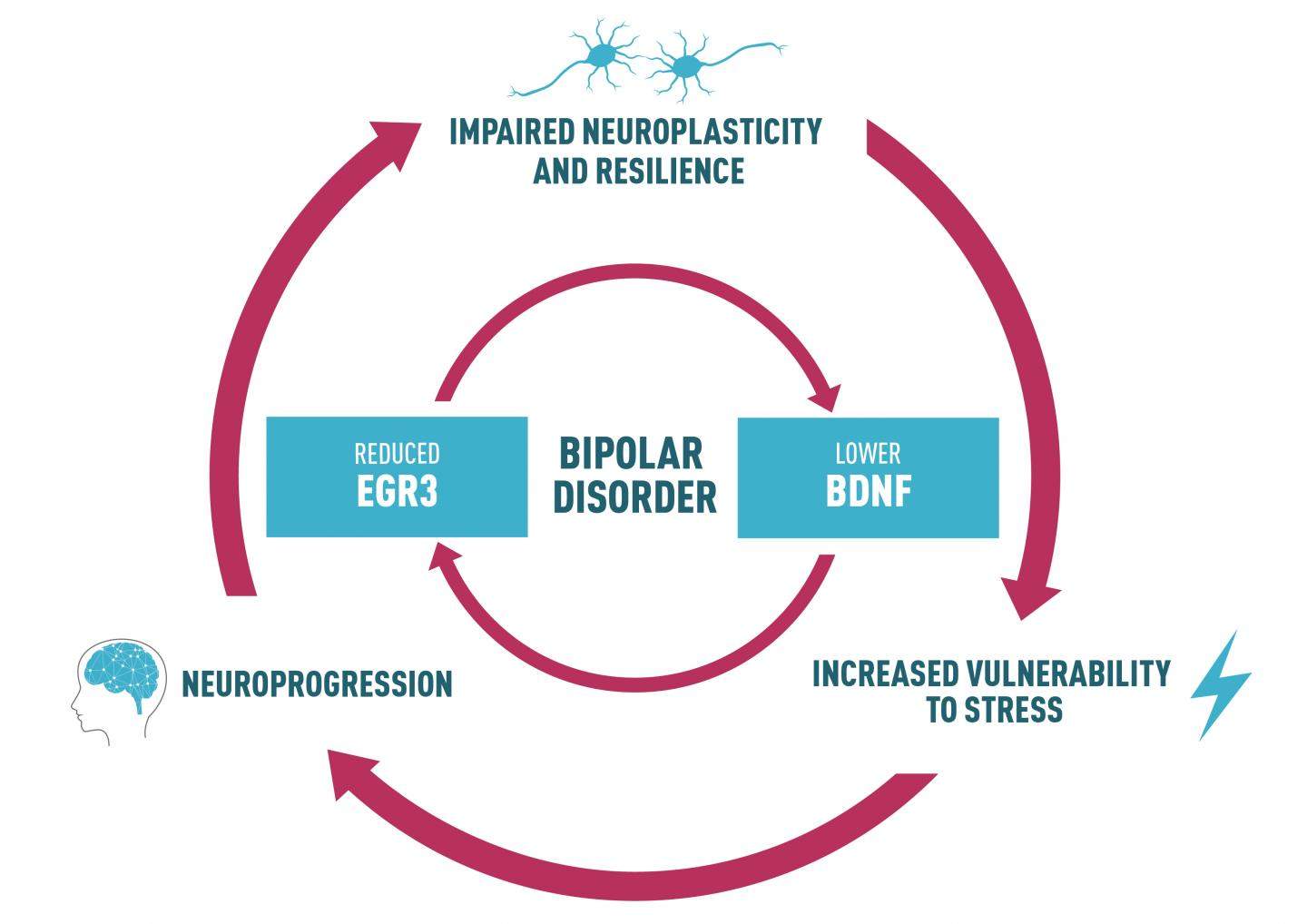
The most recent study by UFRGS and its partners suggests that both EGR3 and BDNF play a central role in BD patients’ impaired cellular resilience. Researchers say that a reduction in EGR3 in BD could lead to a decrease in BDNF levels, impairing patients’ overall resilience and neuroplasticity. This in turn causes an increased vulnerability to stress.
“We believe that the reduced levels of BDNF that has been extensively observed in BD patients is caused by the fact that EGR3 is repressed in the brain of BD patients,” said the study’s lead author and principal investigator at UFRGS Fabio Klamt. “The two molecules are interconnected in a regulatory pathway that is disrupted in BD patients.”
The suggested link between EGR3 and BDNF in BD could prove a potential target for further study and development of new therapeutics.
Study co-author Bianca Pfaffenseller of UFRGS’s Laboratory of Molecular Psychiatry said: “It is possible to imagine that EGR3 may be modulated in order to increase its expression and that of BDNF, which may have a positive impact on BD patients.”
Bipolar disorder treatment
Effective treatment for BD is limited, while finding the appropriate medication and dose proves difficult for each patient. For instance, with mood stabilisers such as lithium the difference between a beneficial and toxic dose is small.
Alternative treatment is starting to gain traction however, with increased research into computerised brain training and bright light therapy. The former treatment tackles everyday problems experienced by BD patients, such as impaired memory and processing functions. The latter is focused on decreasing depressive spells in patients.





