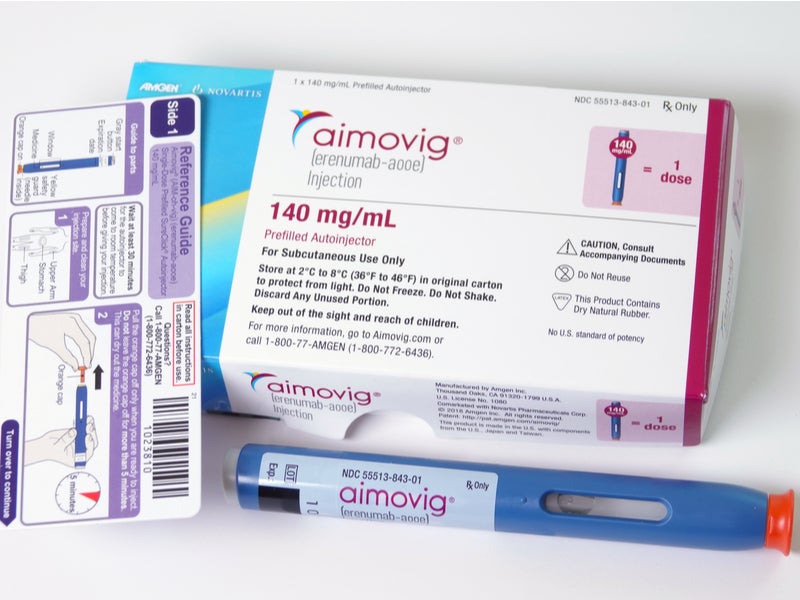
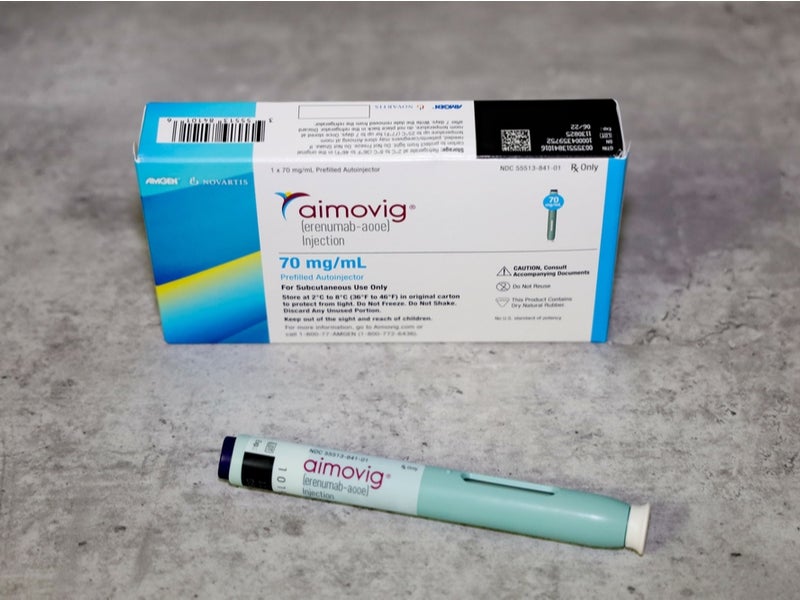
Aimovig™ (erenumab) is a first-of-its-class injectable human monoclonal antibody (mAb) co-developed and co-marketed by pharmaceutical companies Novartis and Amgen for the preventive treatment of migraine in adults.
Aimovig belongs to a class of drugs known as selective calcitonin gene-related peptide (CGRP) antagonists, which is an emerging target of novel migraine therapies.
The US Food and Drug Administration (FDA) accepted the drug’s biological licence application (BLA) in July 2017 and approved the drug in May 2018.
Novartis’ marketing authorisation application (MAA) was accepted for review by the European Medicines Agency (EMA) in June 2017. Aimovig received approval from the European Commission (EC) in July 2018 for the prevention of migraine in adults.
The drug was also registered on the Australian Register of Therapeutic Goods (ARTG) in August 2018 and was approved by Switzerland’s medicines authority Swissmedic in July 2018.
The regulatory applications were submitted following the completion of the pivotal Phase III STRIVE study.
Other approvals for Aimovig
In April 2019, the Scottish Medicines Consortium accepted the use of Aimovig to treat chronic migraine patients whose prior treatment with at least three other preventive medicines had failed.
The UK’s National Institute for Health and Care Excellence (NICE), which reviews the cost-effectiveness of a drug for use on the National Health Service (NHS), declined to recommend the drug in September 2019, judging that it was not cost-effective. NICE’s appraisal committee, however, reconsidered its decision after an appeal and, in March 2021, recommended the drug for preventing migraine in adults who have at least four migraine days each month. This approval came after Novartis submitted additional evidence related to the drug’s cost-effectiveness and clinical efficacy.
The drug is prescribed for migraine prevention on the NHS in Scotland, England and Wales.
In June 2021, the Japanese Ministry of Health, Labour and Welfare approved Aimovig for the suppression of onset of migraine attacks in adults, based on the results of a Phase II study (20120309) and Phase III study (20170609) assessing Aimovig’s efficacy and safety in adult Japanese patients with episodic migraine.
The drug is currently approved in 71 countries, including the UK, Canada and Australia, as well as the European Union.
Aimovig development background
Novartis and Amgen partnered in August 2015 to commercialise and develop neuroscience treatments for Alzheimer’s disease (AD) and migraine. The collaboration focused on several of Amgen’s drugs, including AMG 334 and AMG 301.
In April 2017, the agreement was expanded to include the co-commercialisation of Aimovig in the US.
In April 2019, Novartis filed a lawsuit against Amgen for allegedly trying to terminate their collaboration agreements related to Aimovig, citing breach of material terms as the reason for termination.
The companies later settled their disputes with an amendment in their collaboration agreement in January 2022. Under the amendment, Novartis will hold sole marketing rights to Aimovig outside the US and Japan.
Amgen will discontinue the payment of royalties to Novartis on Aimovig sales in the US. The companies will not share the marketing costs of Aimovig in the US and both firms will continue sharing development expenses worldwide.
Migraine causes and symptoms
Migraine is a neurological disorder characterised by the expansion of blood vessels in the brain due to the release of inflammatory substances from nerves. This results in severe headaches, with symptoms including nausea, vomiting and sensitivity to light or sound.
The root cause of migraine is unknown, but the disorder is believed to occur as a result of a temporary change in the brain chemicals and blood vessels. It may also be caused by hormonal, emotional, physical, dietary and environmental changes, as well as certain other medical factors.
Aimovig’s mechanism of action
CGRP is a protein that causes inflammation in the brain, which may lead to migraine attacks. Its levels rise during migraine pain and subside to normal when pain reduces. Aimovig blocks the CGRP receptor and inhibits the activity of CGRP, preventing the onset of pain.
Aimovig is one of the first fully human mAbs approved for the treatment of migraine. It can be self-administered subcutaneously every four weeks, using a single-dose prefilled SureClick® autoinjector pen containing 70mg/ml solution.
Details of the Phase II clinical study on Aimovig
A Phase II trial named 20120295 was conducted on 667 patients, who were randomised in a 3:2:2 ratio to receive either 70mg or 140mg of Aimovig or placebo.
The randomised, 12-week, double-blind, placebo-controlled study achieved the primary endpoint of minimising the number of migraine days a month in comparison with placebo in both the dosage groups of Aimovig.
Results from the study demonstrated that patient groups of both doses witnessed a mean 6.6-day reduction from an average baseline of 18 migraine days a month, compared with 4.2 days observed in the placebo group.
The drug showed a 50% reduction in the number of days on which acute migraine-specific medication was used, as well as the cumulative hours of headaches, safety and tolerability.
Phase III trials on Aimovig drug
A multi-centre, randomised 24-week, double-blind, placebo-controlled Phase III study named STRIVE was conducted on 955 patients. The patients were given either placebo or subcutaneous Aimovig in 70mg or 140mg doses in a 1:1:1 ratio once a month for six months.
The results of the study showed that patients who received higher doses witnessed a 3.7-day reduction in monthly migraine days from the baseline of 8.3 days. It also showed a reduction in the migraine days by half in 50% of the patients who consumed 140mg of Aimovig, compared with placebo.
With an average baseline of 8.3 migraine days a month, the patients experienced between four and 14 migraine days a month. In the study’s double-blind treatment phase, the patients witnessed a primary endpoint change in the average migraine days each month over the preceding three months.
A Migraine Physical Function Impact Diary (MPFID) assessed the impact of migraines on physical function and everyday activities as secondary endpoints.
The FDA’s approval of Aimovig was based on results from a Phase IIIb clinical study named LIBERTY. This was a multi-centre, double-blind, placebo-controlled study that enrolled 246 patients with episodic migraine, who had had between two and four unsuccessful treatments. The patients were randomised to receive either 140mg of Aimovig or a placebo for 12 weeks.
The trial’s primary endpoint was the percentage of patients with at least a 50% reduction of monthly migraine days from baseline over the last four weeks of the study.
The most common adverse reactions found in patients treated with Aimovig were injection site reactions and constipation.
Patients treated with Aimovig showed significant reductions in the number of migraine days each month during the extensive clinical programme, which involved the participation of 2,600 patients. The drug’s safety and tolerability profile was found to be similar to that of placebo.
The five-year study assessed 70mg and 140mg doses of the drug, which decreased both the number of monthly migraine days and the number of days on which medication for acute migraine is needed.
Data covering 4.5 years from a long-term open-label treatment period (OLTP) showed that treatment with the drug resulted in a 50% reduction in monthly migraine days in 77% of the patients who continued treatment, while 33% of patients achieved full reduction.
Comparative clinical study (HER-MES) of Aimovig against topiramate
HER-MES study is the first and only head-to-head clinical study comparing Aimovig against topiramate. It is a randomised, double-blind, active-controlled, parallel-group Phase IV clinical trial that enrolled 777 adult patients with episodic or chronic migraine in a patient-centred environment.
In the trial, the rate of discontinuation of the treatment due to adverse events in patients receiving Aimovig was 10.6%, compared with 38.9% in patients receiving topiramate.
In addition, 55.4% of patients in the Aimovig arm achieved at least a 50% reduction in monthly migraine days (MMDs) from baseline, compared with 31.2% in the topiramate group.