Cresemba (isavuconazonium sulphate) is an antifungal drug indicated for the treatment of invasive aspergillosis and invasive mucormycosis, which is also known as zygomycosis.
The drug was developed by Astellas in association with Basilea Pharmaceutica International.
Astellas submitted a new drug application (NDA) for Cresemba to US Food and Drug Administration (FDA) for the treatment of invasive aspergillosis and invasive mucormycosis in July 2014. The FDA gave marketing approval for Cresemba for these indications in patients over the age of 18 in March 2015.
Basilea Pharmaceutica International submitted a marketing authorisation application (MAA) for Cresemba to European Medicines Agency (EMA) for the same indications in adults in July 2014.
Disease details of aspergillosis and mucormycosis
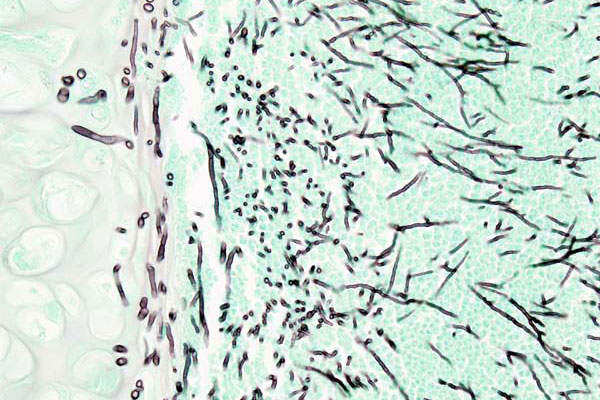
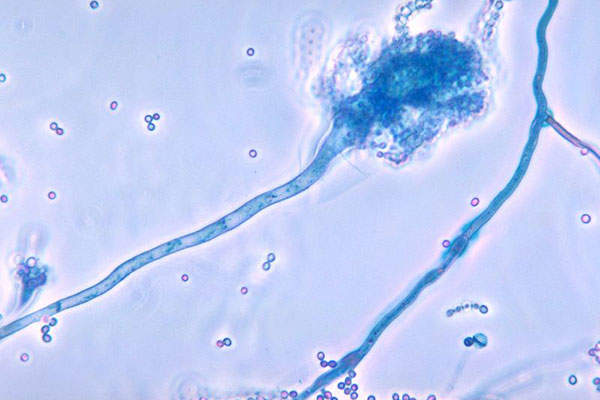
Aspergillosis and mucormycosis are fatal invasive fungal infections. The former is caused predominantly by Aspergillus and the latter is caused mostly by Mucor and Rhizopus fungal species. These infections predominantly occur in immune-compromised patients.
Cresemba’s mechanism of action
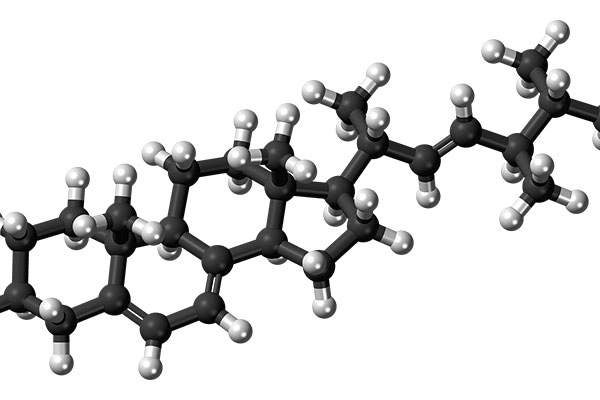
Cresemba contains a triazole antifungal agent called isavuconazole, which targets the cell wall of the fungus and inhibits the synthesis of ergosterol, a key component of the fungal cell membrane.
The drug is available in the form of capsules and injections for oral and intravenous administration respectively.
Clinical trials on isavuconazonium sulphate
Noxafil (posaconazole) is a triazole antifungal agent indicated for treatment of the prophylaxis of invasive Aspergillus and Candida infections.
The FDA approval for the drug was based on results from two Phase III clinical studies known as SECURE and VITAL.
In the SECURE study, 516 patients with invasive aspergillosis or other filamentous fungi were enrolled. The randomised, double-blind, active-control study evaluated the overall safety profile of Cresemba in comparison with voriconazole, another triazole antifungal drug.
Patients treated with Cresemba demonstrated non-inferiority to voriconazole on the primary endpoint of all-cause mortality at day 42. The all-cause mortality reported in the Cresemba treatment group was 18.6%, while it was 20.2% in the voriconazole treatment group.
Adverse events found in the Cresemba-administered patients during the clinical study included nausea, vomiting, diarrhoea, headache, elevated liver chemistry tests and hypokalemia. Some patients also reported constipation, dyspnoea, cough, peripheral oedema, and back pain.
The VITAL study was an open-label non-comparative study intended to evaluate the safety and efficacy profile of Cresemba in patients with invasive mucormycosis. It enrolled a subpopulation of 37 patients with invasive mucormycosis.
Results of the trial demonstrated that all-cause mortality in patients treated with Cresemba was 38%. The efficacy of the drug for the treatment of invasive mucormycosis has not been evaluated in concurrent, controlled clinical trials.
Marketing commentary
Astellas holds the marketing rights of Cresemba exclusively in the US and Canada, while Basilea Pharmaceutica International holds the marketing rights of isavuconazole elsewhere in the world.
Astellas agreed to make a milestone payment of CHF30m ($30m) to Basilea under the license and co-development of isavuconazole. Other medications available for similar fungal infections include Noxafil manufactured by Schering-Plough and Merck.