Developed by Sanofi-Aventis, Acomplia (rimonabant) is a selective CB1 endocannabinoid receptor antagonist indicated for the treatment of obesity. It works by blocking endogenous cannabinoid binding to neuronal CB1 receptors. Activation of these receptors by endogenous cannabinoids, such as anadamide, increases appetite.
Although available in Europe since 2006 for use as an adjunct to diet and exercise for obese or overweight patients with associated risk factors, Acomplia failed to secure FDA approval in the US. Concerns had been growing that patients taking Acomplia (or Zimulti as it was to be marketed in the US) were at increased risk of psychiatric adverse events, including suicidality.
In October 2008, following a review of post-marketing data, the EMEA recommended suspension of the drug’s marketing authorisation on safety grounds. Data had shown a doubling of the risk of psychiatric disorders in patients taking Acomplia in comparison with placebo.
Obesity predisposes to serious illness
Obesity is now the most common nutritional disorder in western industrialised countries. Defined as a body mass index of greater than 30, it arises from the accumulation of excess fat in the body from over consumption of fatty foods.
Prevalence of obesity in the US and Europe has reached epidemic levels.
Data from the World Health Organisation’s MONICA project show that in some parts of Europe over 70% of men aged 55–64 years are clinically obese or overweight (BMI >25) and almost 70% of women in this age group. One in five of all Americans is obese and one in three overweight. Furthermore, increasing rates of childhood obesity are likely to exacerbate the trend towards increasing obesity in adulthood.
There is a strong association between obesity and increased risk of cardiovascular disease and diabetes and possibly certain cancers, such as breast and colorectal cancer.
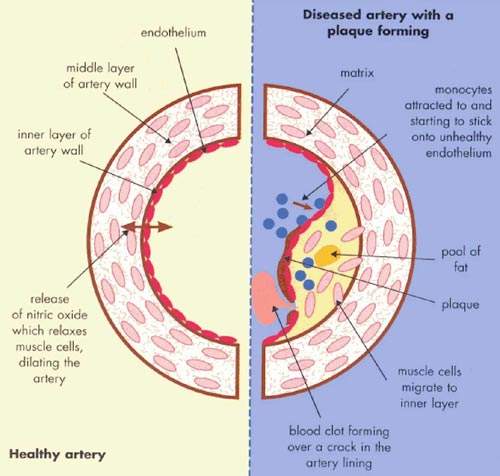
The dramatic rise in the incidence of type 2 diabetes is due largely to the increased prevalence of obesity. Increases in body weight lead to changes in blood lipid and cholesterol levels, predisposing to increased risk of atherosclerosis.
Therapeutic approaches to treatment of obesity
Not surprisingly, the growing prevalence of obesity has stimulated the search for drugs to treat this condition. Various therapeutic strategies have been explored, including:
- Serotonin and noradrenaline reuptake inhibitors (anorectic agents)
- Lipase inhibitors
- ß 3-adrenoreceptor agonists
- Leptin agonists
- Melanocortin-3 agonists.
Sanofi-Aventis’ approach is completely different to the above. It developed from the knowledge that cannabis smokers often experience extreme hunger pangs, which cannabis smokers refer to as "the munchies". Sanofi-Aventis worked on the premise that if cannabinoids stimulate appetite, blocking cannabinoid receptors in the brain might reduce appetite.
The central cannabinoid (CB1) receptors are believed to play a role in controlling food consumption and the phenomena of dependence / habituation. To develop suitable drugs against this target, the human cannabinoid receptor was first cloned and then expressed in cells.
Compounds with potential inhibitory activity against this receptor were then screened for inhibitory activity. Rimonabant emerged from this screening process as a potent CB1 receptor antagonist.
Preclinical animal studies subsequently showed that it could reduce consumption of fats and sugars, which contribute to weight gain.
Phase III data highlight efficacy
The promising preclinical findings with Acomplia (rimonabant) have been confirmed in a series of clinical studies, including pivotal phase III trials involving over 6,000 obese subjects that were carried out in both the US and Europe.
Two-year data from the phase III multicentre Rimonabant In Obesity (RIO) trials, which compared rimonabant at doses of 5mg and 20mg with placebo with respect to weight reduction and prevention of weight gain, showed that the positive results seen after a year’s treatment were sustained over the full two-year trial period.
Consistent with the one-year data, the results showed that overweight and obese patients taking rimonabant 20mg/d achieved significant reductions in body weight, waist circumference (an indicator of abdominal obesity) and improved lipid and glycaemic profiles compared with placebo recipients. Rimonabant also had a significant impact on metabolic CVD risk factors, greater than that expected by weight loss alone.
Efficacy and safety in long-term use is important feature of any anti-obesity drug. Some potential anti-obesity medications have proved effective in the first six months of treatment only to lose effectiveness as subjects develop resistance to treatment.
Long-term safety is also a major concern. In the US, the FDA generally requires two years of safety data before approving antiobesity drugs. Results from the phase III RIO trial programme had suggested that rimonabant was well tolerated in long-term use.
However, an FDA meta-analysis of rimonabant safety data indicated an increased risk for suicidal ideation in patients on the highest 2mg dose: two suicides were recorded across the rimonabant clinical trial programme, one of which occurred in the RIO-North America trial.
The FDA committee also expressed concerns about an increased risk of other psychiatric adverse events and adverse neurological events including seizure with rimonabant 20mg, while noting the high numbers of patients who withdrew prematurely from the RIO trials during the first year of treatment. In Europe, the EMEA has now taken a similar view.
Marketing commentary
The market for weight-reducing drugs has had a somewhat chequered history, characterised by major product withdrawals. Although the statistics suggest a market with enormous opportunity, pharmaceutical companies have so far been unable to capitalise on the need for anti-obesity agents.
Only two drugs are approved for long-treatment of obesity. They are the lipase inhibitor orlistat, the leading medicine for weight reduction, and sibutramine. Use of both products has been limited by side effects.
In the prevailing market there is a clear opportunity for an effective and well-tolerated anti-obesity drug. Although Acomplia (rimonabant) appeared efficacious, like previous anti-obesity drugs, safety issues have led to its withdrawal.