Simon Robertson, a former video game developer, first tried on a virtual reality (VR) headset back in 2012 and immediately started thinking about how the technology could be applied to help people.
That night, he fell into a research rabbit hole where he discovered the work of Dr Hunter Hoffman, one of the originators of a new technique using immersive VR for pain control.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Hoffman was able to show that burn patients, while having their wound dressings changed, were reporting significant pain reduction while being immersed in VR.
“I was really impressed by this research but disappointed to discover that interactive, immersive distraction wasn’t being used at burn centres and paediatric hospitals,” says Robertson. “So, I kind of made that my mission.”
The road to KindVR

Robertson hauled his old computer and clunky VR headset to Oakland Children’s Hospital, now called the UCSF Benioff Children’s Hospital Oakland, and excitedly presented his findings.
They were struck by the research but told Robertson to “slow down” and had him become a child life specialist volunteer. He spent about a year working bedside with haematology patients, mostly those suffering from sickle cell disease. At this time no VR was involved. Instead, Robertson used the opportunity to get a sense of the common procedures that these patients go through and imagine what integrating VR to help them would look like.
From there, Robertson partnered with Dr Anne Marsh, director of the Paediatric Sickle Cell Clinic and associate haematologist/oncologist at UCSF Benioff, who became the primary investigator on the first clinical trial for KindVR – the VR therapy firm Robertson founded in 2014 – looking at harnessing VR for sickle cell inpatients during vaso-occlusive pain crises.
Patients with sickle cell disease are burdened with excruciating episodes of pain and often require hospitalisation for intravenous opioids to help relieve it. Opioids, although necessary for episodes of intense pain, often are not sufficient and come with a myriad of other problems like addiction, adverse reactions and declining long-term efficacy.
In the UCSF Benioff trial, Robertson and Marsh enrolled a convenience sample of 30 sickle cell patients aged eight years or older, all of whom were admitted with a vaso-occlusive pain episode.
Results showed pain intensity dropped significantly after a single VR session, with improvements in sensory, affective, evaluative and temporal pain domains. The use of the VR sets, which were programmed with KindVR Aqua, a calming virtual underwater world, was very well received by patients, parents and hospital staff.
KindVR now has 10 clinical trials underway with 10 leading hospitals and three trials that are completed and published. Other indications where KindVR’s tech is being trialled include a variety of cancer procedures, laceration repair, preoperative stress, MRI practice and IV insertion.
Distraction as pain mitigation
Robertson says VR’s ability to reduce pain and stress all comes down to distraction –directing patients’ attention to a virtual world leaves a little less bandwidth for the brain to process the pain signals that go up the spine.
“The truth is, distraction is something that’s been known by providers and parents for many years,” Robertson says. “My first day working in Oakland Children’s I saw child life specialists use a vibrating pillow on the side of the patient, asking them to focus on that physical sensation while they did a difficult procedure on the opposite side of this patient’s body while simultaneously playing a game of I Spy – a more cognitive form of distraction.
“I was watching this kiddo be distracted on two fronts, and it became clear to me that that’s the magic of VR. It’s not necessarily a panacea, it just happens to be a little bit better at hijacking the brain senses, by controlling what you see and hear and your sense of presence in the environment. It pulls you out of that hospital. Really that just adds up to a more effective distraction technique. I see VR as just another step forward in being able to distract patients from processing that pain, and giving them something to look at.”
VR worlds tailored for patients and CROs
KindVR has a number of ‘worlds’, or applications tailored specifically to the hospital setting. When we think about VR, we normally imagine exciting immersion where the wearer might experience riding a rollercoaster or being chased by a T-Rex. While these situations sound fun, they are not suitable for a patient in hospital who is having an IV insertion or using very powerful medication to manage their pain.
“Patients deserve access to software that’s designed for their specific patient population or the procedure they’re going through,” says Robertson. “That was the foundation for me as a designer, to design for these procedures.”

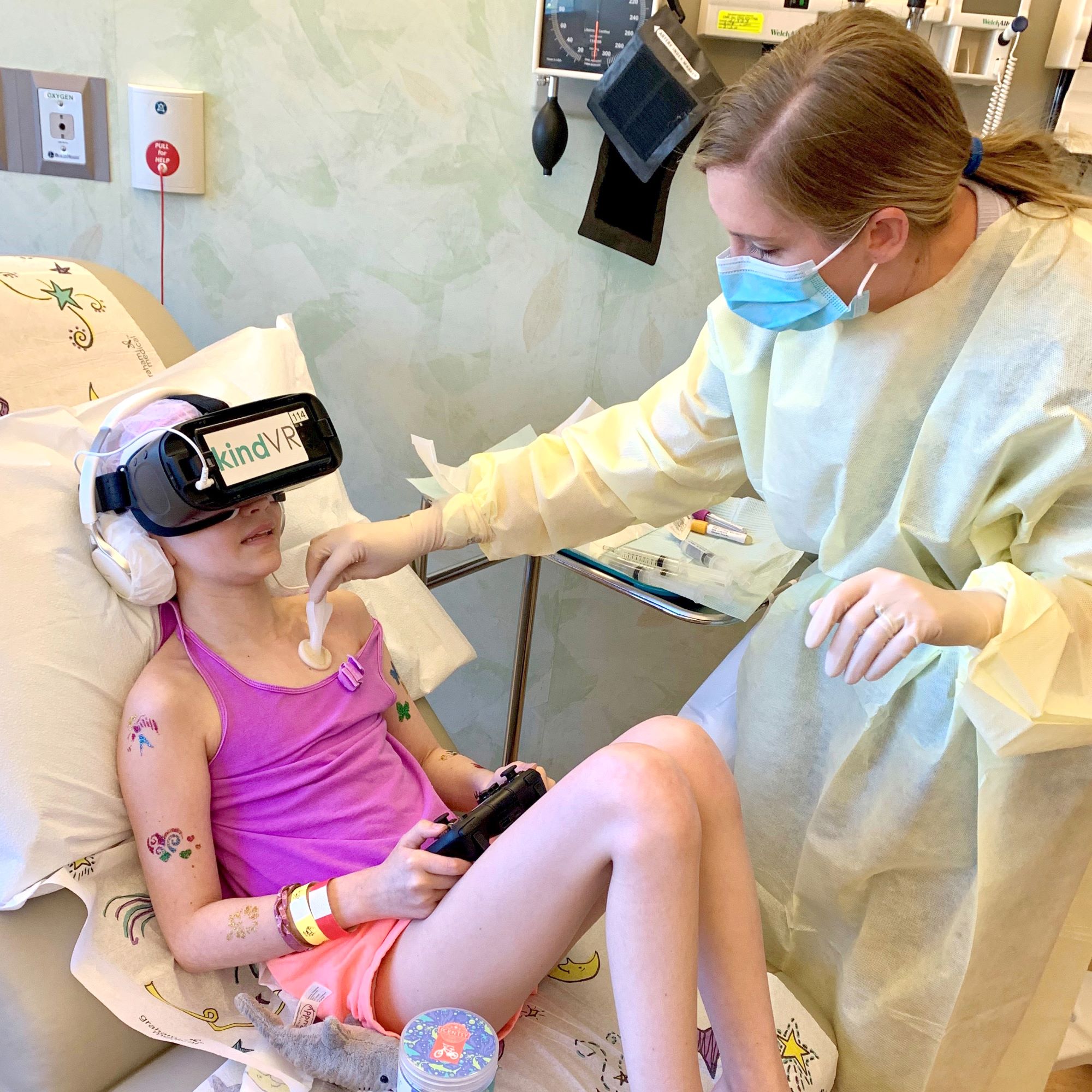
Image Credit: KindVR
Aqua is KindVR’s main application for acute pain and stress, an underwater adventure where patients interact with whales and dolphins and play a very simple game. It’s designed to be used from a hospital bed or a wheelchair, as patients may have restricted mobility. They find themselves in a little submarine that acts as a safe space while they interact with the environment and also encourages them to face forward in their seat and keep still. This can help increase safety and reduce pain and stress in a number of hospital procedures.
KindVR’s clinical trial at the Hospital for Sick Children in Toronto looks at port access procedures – a common procedure for oncology patients for chemotherapy delivery. Robertson created a custom version of Aqua designed for patients to lay back, being either supported by their parents, or at about 45 degrees in their chair.
Patients play a version of the game where all the visuals in the underwater world are just above eye level, meaning that the patient will naturally assume a position that is perfect for the nurse to carry out the procedure.
“We found it really can reduce the pain in the procedure but also that pre-procedural anxiety and anticipatory pain that goes with it,” Robertson says.
KindVR provides a complete solution for the hospitals and contract research organisations (CROs) they are involved with. They run clinical trials with all partner hospitals on each application to ensure that they are validated for safety and efficacy.
The headsets are wireless and don’t rely on the internet, nor do they collect patient data and are HIPAA-compliant.
Pre-Covid, KindVR would visit each hospital to train staff on how to use the hardware but over the past year, this training has been done via Zoom.
Improving patient retention
Robertson says the use of VR technology in clinical trials can aid in patient recruitment and retention. Participating in a clinical trial or enrolling a child is a big decision that often requires a long commitment involving some very difficult days of pharmacokinetic (PK) testing and blood draws. These procedures can bring a lot of anxiety both on the day and leading up to it.
“We really think being able to provide a headset as a pain mitigation and anxiety-reducing tool can really encourage patients to enrol,” says Robertson.
“This is especially true for children, who we think have to go through some of the most gruelling procedures out there. If we can take that first moment of extreme anxiety, pain and stress and prevent it by allowing the patient to escape into a virtual world, we can change that patient’s relationship with the hospital.”
Robertson says the hospitals he collaborates with have received many reports of patients that used the KindVR headsets saying they were happy to go back to the hospitals associated with such a positive experience. “That’s really where we’re hoping to get to, both for our clinical trials and our daily-use hospitals.”
Robertson has found that another outcome of using VR is that it has been of huge value to parents and providers as well as patients.
“Providers love integrating VR when they do difficult procedures because they don’t have to be as much of a villain,” he says. “Parents email me frequently talking about having to hold their own child down during difficult procedures, and often VR changes that entirely. Some of these parents report that their child doesn’t even notice the procedure when it’s happening.”
From the provider perspective, there are also benefits when it comes to saving time and money. Robertson said that some of KindVR’s future trials will be looking at just that.
“With some more stressful or painful procedures that can cause a patient breakdown, a 10-minute procedure can take an hour – that’s where VR might help accelerate some things.”
Future of VR and decentralised trials
Robertson says KindVR has had incredible success with needle pokes, burn wound dressing and laceration repair and the company is now looking to target reducing pain and stress in more complicated procedures, including catheter placements, cranial nerve block for patients with migraines and lumbar punctures. Additionally, the company will be looking at using the headsets to prep patients for MRI scans and for treatment in rehab.
“There’s no shortage of procedures for us to look at and as headsets get lighter and easier to use, I think some of the hardware is going to fade away and will become more about patients being able to manage this on their own and have these as effective and safe validated tools,” Robertson says.
Looking towards the increasingly prevalent decentralised clinical trial approach, KindVR currently has a paediatric study in development with an unnamed CRO targeting a rare disease and wanting to reduce the number of times patients have to go to the hospital to participate. KindVR is planning to send VR headsets to the families, who will use them while home health nurses conduct blood draws.
“I’m really proud to be able to look at these design challenges and be at this really interesting intersection of interactive technology and healthcare,” says Robertson.
“I think there’s no limit of where this can go in terms of improving patient lives, and I’m really hoping that more hospitals will continue to take time to integrate this and that CROs and pharma companies will continue to see its value too. Over the next five years, I think this technology will become more and more commonplace.”





