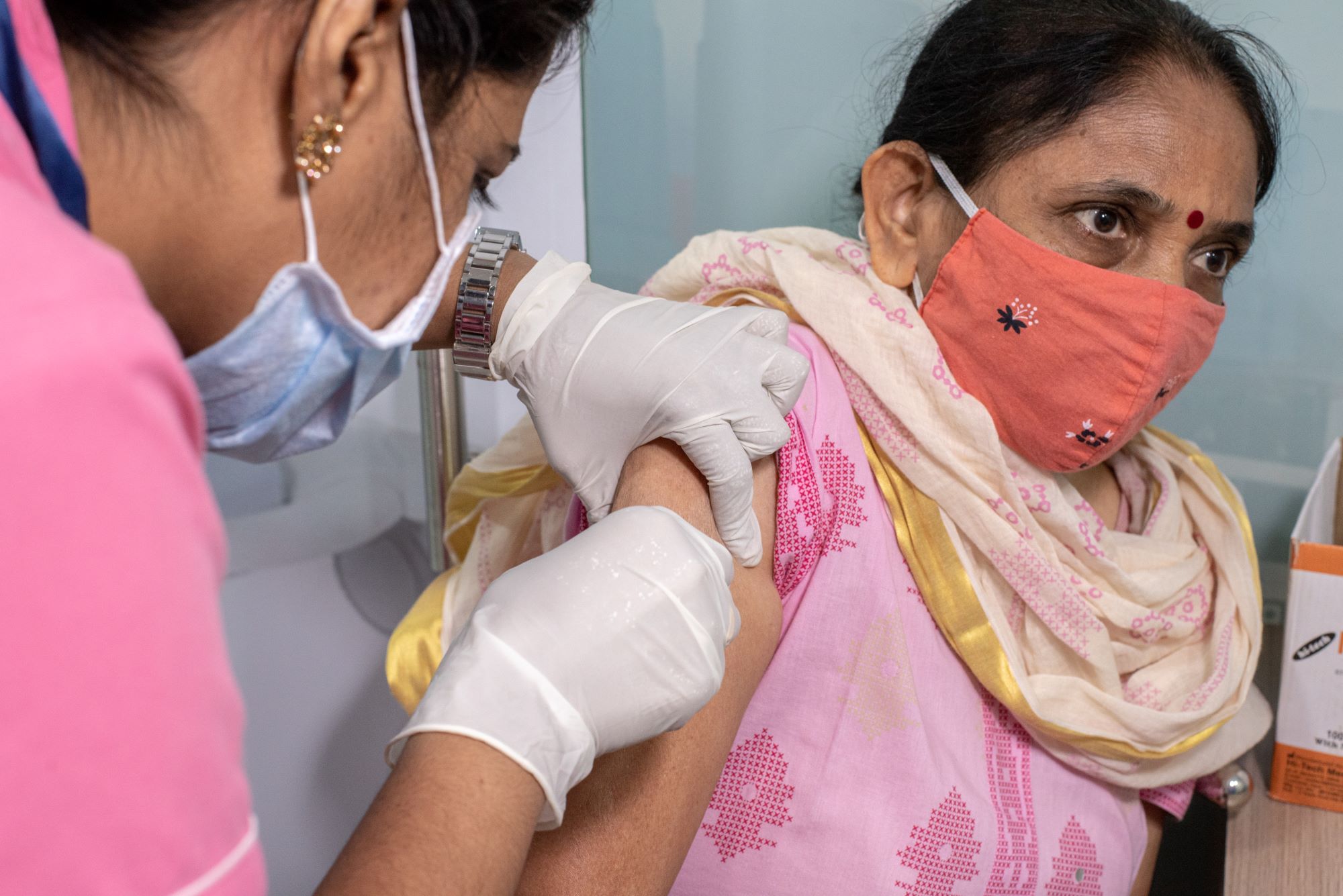
India’s Bharat Biotech has finally announced interim Phase III data for its Covid-19 shot, with the vaccine showing 78% efficacy at preventing mild, moderate and severe coronavirus infections and working well against most variants.
Bharat’s second interim analysis is based on accruing more than 87 symptomatic cases of Covid-19. Due to India’s recent surge in cases, 127 symptomatic cases were recorded, resulting in a point estimate of vaccine efficacy of 78% (95%CI: 61-88) against mild, moderate, and severe Covid-19.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Covaxin, India’s first domestically-developed Covid-19 vaccine, is a two-dose jab that uses an inactivated or “dead” form of the virus. The shot also showed 100% efficacy at preventing severe Covid-19 and hospitalisations, according to a joint statement from Bharat and co-developers, the Indian Council of Medical Research (ICMR).
The vaccine’s Phase III study enrolled 25,800 participants between 18-98 years of age with 10% of participants being over the age of 60. Analysis was conducted 14 days after the second dose.
“Efficacy against SARS-Cov-2 has been established,” said Bharat Biotech’s chairman and managing director Dr Krishna Ella. “Covaxin has demonstrated an excellent safety record in human clinical trials and in usage under emergency use.”
“Covaxin is now a global innovator vaccine derived from research & development from India. The efficacy data against severe Covid-19 and asymptomatic infections is highly significant, as this helps reduce hospitalisations and disease transmission, respectively.”
The data has yet to be peer-reviewed and a final analysis will be available from June, according to the company.
Several million doses of Covaxin have now been supplied and administered in India and several other countries.
Covaxin controversy
Covaxin has been a subject of controversy among health experts within and outside India since it was announced in January that Bharat’s candidate had received emergency use approval from India’s leading drug regulator, the Central Drugs Standard Control Organization (CDSCO). This authorisation came before the vaccine had completed Phase III trials in humans or published data on Phase II trials.
The CDSCO used hazy language that left the scientific community somewhat perplexed – the regulator stated that Covaxin had been approved for “restricted use in an emergency situation” and that it would be rolled out in “clinical trial mode”.
The decision was criticised widely for its hastiness and lack of transparency, leading to accusations of the approval being driven by a mixture of political pressure and the competitive nature of Bharat Biotech.
“Both things are aligning here,” said Prashant Yadav, a healthcare supply chain expert at the Centre for Global Development in Washington. “Government pressure and the company’s internal competitive drive.”
Back in January, the All India Drug Action Network said, as reported by the BBC, that it was “baffled to understand the scientific logic” to give the nod to “an incompletely studied vaccine” and said that there were “intense concerns arising from the absence of the efficacy data”.
“The phases of a vaccine or a drug trial have historically evolved from the need to protect individuals from both vaccines/drugs that may not be effective when tested in large populations, and those that may harm individuals as a result of rarer adverse reactions that will only be evident when a large number of individuals are tested,” said Consultant Pulmonologist, PD Hinduja Hospital & MRC Dr Lancelot Pinto.
“Bypassing these phases would be jeopardising a system which has been created and has evolved to protect individuals.”
The criticism sparked a number of knee-jerk emotional media responses from Bharat’s chairman. “Indian companies are targeted by everyone in the world,” Ella said during a January press conference. “It hurts us as scientists – we don’t deserve that type of bashing.”
When the vaccine began to be administered to health workers on the heels of the controversial approval, many revolted, saying they didn’t want to receive a vaccine that had not undergone the standard approval and trial process. Many said they would rather receive Covishield, AstraZeneca’s vaccine being produced in India by the Serum Institute of India (SII), which received approval in the country at the same time as Covaxin.
Which vaccine front-line workers received was a lottery but odds were on them receiving Covaxin, which Dr Dayanand Sagar, the Bengaluru-based president of a resident doctors’ body said they were being “compelled” to take.
Trial concerns at The People’s College
As well as complaints around the opacity of Covaxin’s emergency approval process, questions have also been raised about the running of the vaccine’s all-important Phase III trial. The People’s College of Medical Sciences and Research Centre in Bhopal, one of the 26 sites at which Covaxin’s Phase III trial took place, has been accused of not following proper procedures while screening candidates and collecting data.
There was even talk of the hospital flouting informed consent protocol with many of the trial participants (900 of whom came from vulnerable backgrounds) reportedly being rounded up into vehicles and not knowing that they were taking part in a clinical trial at all. Many claimed to not receive a copy of their consent form, even after getting their first dose.
Many of those vulnerable participants were illiterate and therefore supposed to have access to an audio-visual recording for informed consent, but participants have come forward saying that no such recordings were made.
There were also claims of coercion as trial participants were being offered Rs750 ($10) for each visit to the trial site. Activists accused Bharat of using remuneration to get poor participants to take part in a trial that was struggling to attract volunteers, but the firm stated that the sum was for reimbursement and was “approved by every Institutional Ethics Committee (IEC) at the study sites”.
People’s College said it had put a system in place to follow up with patients every day for seven days following administration of the first dose. However, this data collection has been described as “extremely chaotic” and many of the trial participants claimed they were not contacted each day, and some not at all, meaning that the data around any adverse events from this site may have been tainted.
Additionally, some patients that felt ill after receiving the vaccine went back to the hospital for treatment and were asked to pay or were turned away.
To make matters worse, in December there was one case of death in a patient who had received the vaccine in the Phase III trials, although Bharat affirmed this was not down to its vaccine but in fact due to some unspecified poison the patient had consumed. Critics have argued that this certainty was completely unwarranted, especially as the patient’s family had a very different version of events, stating that the patient became ill soon after receiving the vaccine.
Also marring The People’s College’s certainty is that it has said that the trial investigators and ethics committee continue to be blinded, meaning they did not know if the patient received the vaccine or a placebo. This would have been the only quick way to ascertain that the vaccine did not cause the death – if the patient had received the placebo.
Does Covaxin protect against mutant strains or not?
There is also some uncertainty and mixed messaging around Covaxin’s efficacy in protecting against various strains of Covid-19 and the multiple mutated variants recently found in India.
In last week’s announcement of the second interim Phase III data, ICMR director general Professor Balram Bhargava, said he was happy to note “that Covaxin works well against most variants of SARS-CoV-2.”
On the same day, the ICMR tweeted: “ICMR study shows Covaxin neutralises against multiple variants of SARS-CoV-2 and effectively neutralises the double mutant strain as well.”
However, just a day before, Ella told NDTV there is “no information yet” on how well Covaxin might work against Covid variants.
A country in great need
India is now facing a terrifying volume of new cases and has the second-highest number of reported cases globally after the US. Currently, cases in India are rising at a catastrophic rate of 300,000 per day.
The South Asian nation is now under attack by a new ‘double mutant’ form of the virus, which was first detected in Maharashtra’s Nagpur in December last year and has now spread to 18 states.
India has 1.3 billion people to vaccinate across remote villages and densely populated cities. Regardless of the controversy affecting the reputation of Covaxin, the vaccine will likely be imperative to getting India out of this desperate situation.
Despite the damaging accusations that have been made about Bharat Biotech and its vaccine, the firm has a great track record for bringing safe and effective original vaccines to market, with 16 vaccine approvals in its portfolio.
Currently, the only other option for a vaccine available to Indian citizens is Covishield, the SII-produced version of the Oxford/AstraZeneca vaccine. While the lack of transparency around Covaxin’s testing and approval have been a cause for concern, the latest interim data is encouraging and India is urgently in need of an abundant and affordable vaccine to build on the Covishield vaccination programme.
Last week, Bharat Biotech announced it had ramped up its manufacturing capacity to produce 700 million doses of Covaxin per year.
“Last month we produced 15 million doses, this month we are reaching 20 million doses, next month we will be making around 30 million doses followed by 70 to 75 million doses,” Ella said. The company expects to reach a production capacity of up to 800 million doses a year by August. With India’s Covid-19 surge sowing chaos in the country’s embattled healthcare system and jeopardising the global vaccination drive, it’s vital that Bharat moves quickly to clarify Covaxin’s safety and efficacy data so that a speedy rollout can proceed with confidence.





