Pfizer’s Phase III Rivipansel (GMI-1070) Evaluating Safety, Efficacy and Time to Discharge (RESET) pivotal trial has failed to meet its primary or key secondary efficacy endpoints.
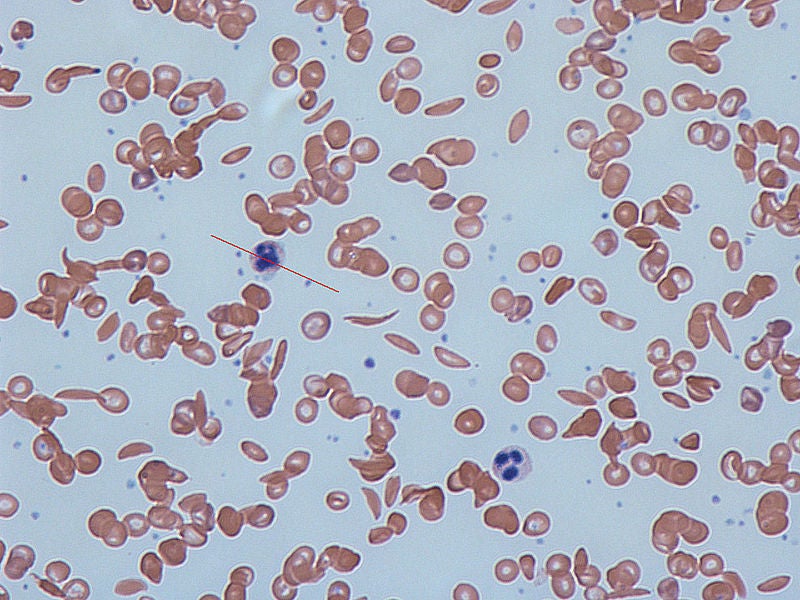
The trial aimed to assess the efficacy and safety of rivipansel for the treatment of patients aged six and older with sickle cell disease (SCD), a debilitating blood disorder.

Discover B2B Marketing That Performs
Combine business intelligence and editorial excellence to reach engaged professionals across 36 leading media platforms.
Readiness-for-discharge was the trial’s primary endpoint, while the key secondary efficacy endpoints were time-to-discharge, cumulative IV opioid consumption, and time to discontinuation of IV opioids.
Pfizer Global Product Development Rare Disease senior vice-president and chief development officer Brenda Cooperstone said: “We are disappointed with the results, as we have been working in close partnership with the SCD community to advance rivipansel as a potential treatment option for acute VOC.
“We plan to share the study data at an upcoming scientific meeting as we want to ensure the learnings from this trial help inform future sickle cell programmes that aim to improve care for SCD patients experiencing a VOC.”
The multi-centre, randomised, double-blind, placebo-controlled, parallel-group RESET (B5201002) trial included 345 patients with SCD aged six and older experiencing a vaso-occlusive crisis (VOC).
Patients in the trial were randomised 1:1 to receive rivipansel or placebo, administered intravenously every 12 hours up to a maximum of 15 doses.
Post randomisation, all study participants were followed for 35 days after their last dose of the study drug.
Pfizer chief patient officer and executive vice-president Freda Lewis-Hall said: “We recognise this is a significant setback for the SCD community, who are eagerly awaiting new treatment options, and we share in their disappointment.”
After completing the RESET trial, eligible patients could enter an open-label extension study (B5201003) and receive rivipansel for subsequent VOC episodes for 18 months.
Last month, Pfizer’s Phase III trial of intravenous (IV) sildenafil (Revatio) added to inhaled nitric oxide (iNO) to treat newborns with persistent pulmonary hypertension (PPHN) failed to achieve its primary efficacy endpoint.





